Walk-ins rarely arrive in a neat sequence. A missed hearing, a housing crisis, a custody issue, and a routine question can hit your front desk within minutes. Without an intake triage standard for legal intake, your staff improvise, urgency gets read differently, and fairness starts to drift.
You don’t fix that with more effort. You fix it with a shared triage system, clear ownership, and a fast way to decide what happens next. That starts with a standard your team can use on its busiest day.
Key takeaways
- A walk-in intake triage standard protects fairness in your triage system, not only speed.
- Your standard should define prioritization criteria for urgent cases, minimum data, next-step codes, and handoff ownership.
- You can start with paper, a shared sheet, and a short script before you change software.
Why a walk-in intake triage standard matters
When walk-in volume rises, much like in an emergency department, the problem is not only speed. The bigger issue is inconsistency. One staff member treats a same-day deadline as urgent. Another books it for later. Someone else tries to solve everything at the desk, which slows the whole line.
That variation has a real cost. It disrupts the decision-making process and harms resource allocation. Clients repeat their story. Staff burn time on avoidable back-and-forth. Leaders lose visibility because each exception lives in a notebook, inbox, or memory. Meanwhile, privacy risk grows when sensitive facts land in the wrong place.
A good standard gives you one definition of urgent, one minimum data set, and one owner for the next step. It improves workflow efficiency and makes the front door calmer. If requests still arrive through several request channels, a single front door intake guide can help you tighten intake before the queue gets worse.
Legal aid teams have documented structured triage for years. You can see that logic in Illinois Legal Aid Online’s triage documentation and broader online intake resources from the Legal Aid Association of California. The lesson is clear. Triage works when the rules are shared, short, and easy to follow under pressure.
Triage is a fairness tool. It helps you route people by need and time risk, not by who asked loudest.
What your intake triage standard should include
Your standard does not need to be long. In fact, long standards usually fail at the front desk intake process. You need a one-page rule set that staff can apply in under three minutes.
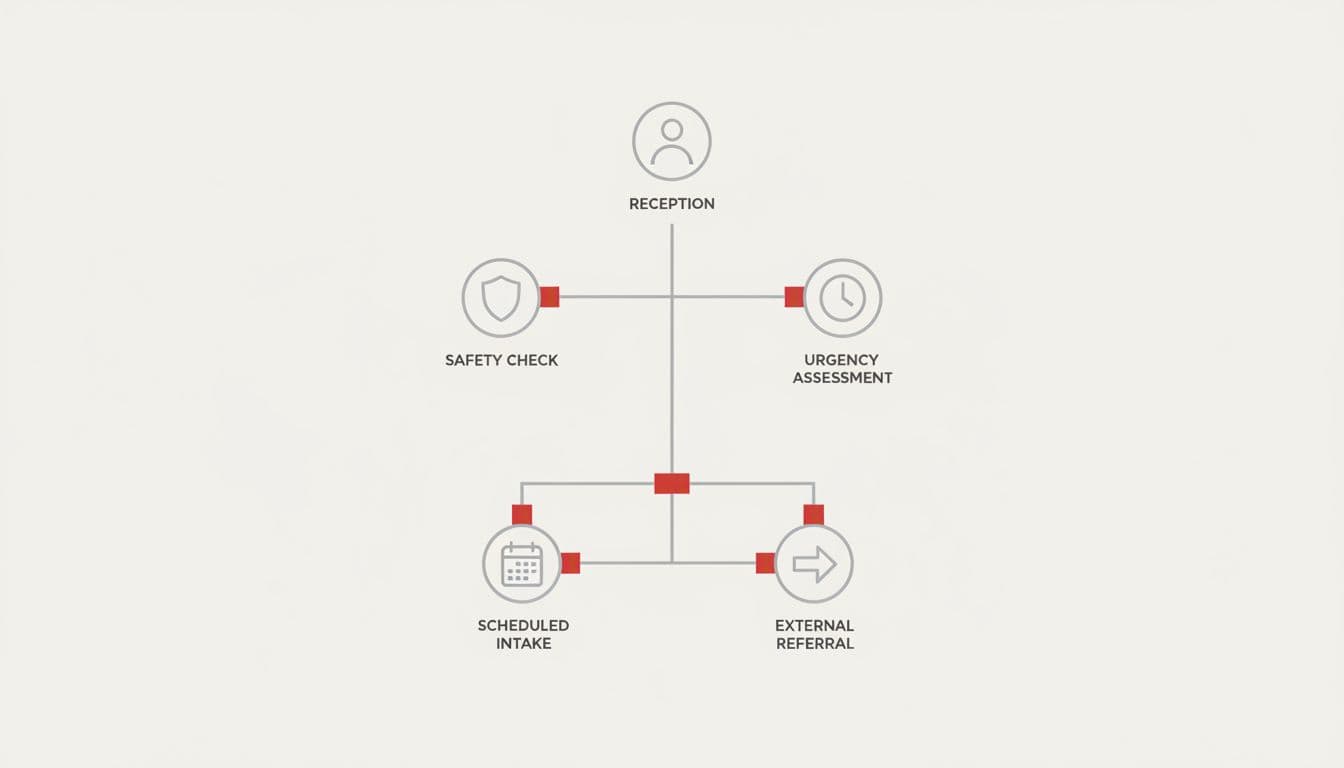
Start with four pieces. First, define the minimum data you must capture before routing using standardized forms. That often means name, safe contact method, issue type, deadline risk, and any immediate safety concern. Second, define a quick safety check. If someone faces imminent harm, the case leaves the normal queue at once. Third, define triage categories. Fourth, define what counts as a complete handoff, including the decision owner for scoping and resourcing.
Here is a simple triage algorithm that outlines the tier definitions by level of acuity:
| Tier | Use when | Target action |
|---|---|---|
| Urgent | Deadline, safety risk, loss of liberty, active court event | Same day |
| Priority | Time-sensitive problem, but not same-day critical | Within 1 to 3 business days |
| Routine | General information or lower time risk | Scheduled next step |
The table matters because it turns instinct into policy. Now your staff can make the same call, even on a crowded afternoon.
Your standard should also name a short set of next-step codes, such as “scheduled,” “warm transfer,” “referred out,” or “needs callback.” That language matters for reporting. If every person uses different terms, your numbers stop meaning much.
Finally, define “handoff complete.” A referral is not complete when you hit send. It is complete when the receiving party confirms receipt, or your team records the next verified step. That is where a closed-loop referral playbook becomes useful, especially when walk-ins move to outside partners.
How to put the standard in place without slowing service
You do not need a system overhaul to start. Most teams can pilot a workable intake triage standard using a simple two-week workplan. Begin with one site, one script, and one owner per shift. Through stakeholder engagement, train staff on the same examples, especially edge cases like partial information, language access needs, and urgent walk-ins near closing time.
Keep the first version simple. Log exceptions instead of arguing over them in real time. Then review those exceptions once a week using engagement protocols. That is where the standard gets better. If the same issue keeps breaking the flow, change the rule or clarify the script.
Measure only a few things at first. Track time to first response, percent of urgent matters handled within target, incomplete handoffs, and cases that sit without a next step. If leadership needs to build strategy capacity in legal operations, the intake-to-outcome clarity checklist helps you spot bottlenecks before they harden into routine.
If you already use a legal aid triage tool, your task is still the same. You need shared definitions, not only software settings. The OTIS management guidance is a useful reminder that triage logic only works when teams manage it with discipline.
FAQs about walk-in intake triage
Is triage the same as eligibility screening?
No. Triage decides the next step and the time frame, distinct from routine screening. Full eligibility review can happen later if the case moves forward.
How do you handle urgent walk-ins with limited information?
Like clinical decision-making in disaster triage, capture the minimum facts for potential life-saving interventions, move the matter out of the normal queue, and document the reason for escalation. You can fill in the rest once the immediate risk is addressed.
Do you need new software to create an intake triage standard?
No. Many teams start with a paper form, a shared sheet, a short routing script, or a self-service portal. Process clarity should come before tool changes.
What should leadership review each month?
To align with the enterprise agenda and fulfill their mandate, ask for a short report with time to first response, urgent matters met on time, open referrals without confirmation, and top reasons cases stall. Those four measures reveal a lot.
A strong intake triage standard does not make demand disappear. It gives your team a calmer, fairer way to handle it, streamlining the intake process. When the rules are clear, staff stop guessing, clients get clearer next steps, and leadership gets visibility it can trust.
Start small, keep the standard short, and refine it from real cases, focusing on the decision moment and defining clear triage categories. That is how you move from front-desk chaos to confident decisions.

